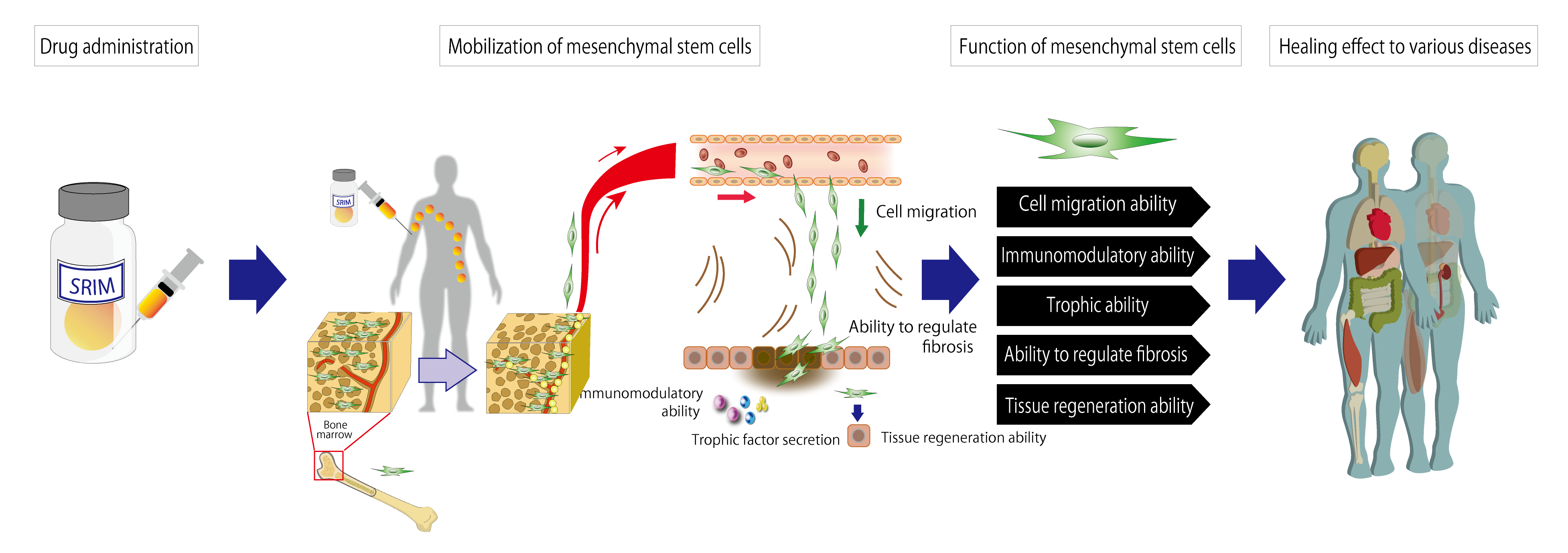
PJ1: “Regeneration-Inducing Medicine™” HMGB1 peptides (Redasemtide)
These are peptide formulations created from the bioactivity domain of the biologic protein HMGB1. When administered intravenously they mobilize the mesenchymal stem cells in the patient’s bone marrow into peripheral blood, and accumulate them at the site of damage, promoting tissue regeneration and healing of the affected site. Since the mesenchymal stem cells mobilized into the damaged tissue by the medicine directly treat the damaged tissue, a single substance is expected to have a wide range of indications, due to the characteristics of mesenchymal stem cells, which include cell migration ability, immunomodulatory ability, trophic ability, ability to regulate fibrosis, and tissue regeneration ability. In non-clinical pharmacological studies using animal disease models conducted up to the present, good therapeutic effects have been confirmed for diseases including cerebral infarction, myocardial infarction/cardiomyopathy, epidermolysis bullosa, intractable skin ulcers, spinal cord injury, amyotrophic lateral sclerosis (ALS) and traumatic brain injury. Since the compound administered is a substance such as a peptide or protein, it can be manufactured, transported, stored and administered by the same methods as conventional medicines. This means that while this treatment resolves various issues relating to regenerative therapy and cell therapy, it can target the treatment of diseases that were difficult to treat with conventional therapies.
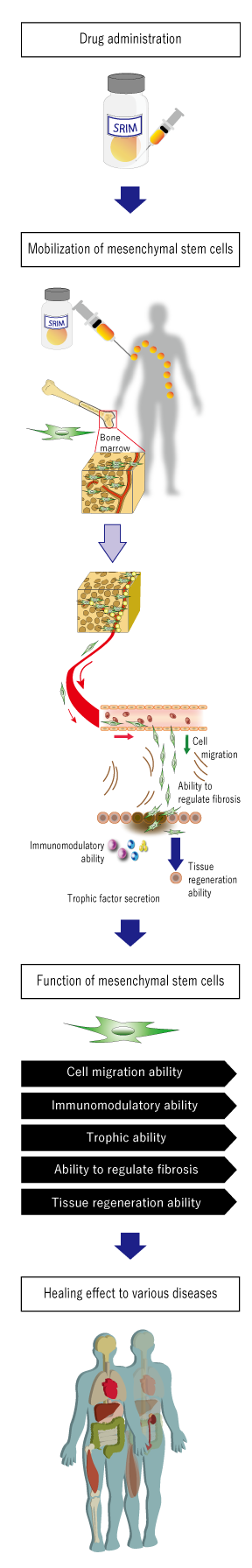
PJ2: Novel Regeneration-Inducing Peptide for Systemic administration
Since our discovery of regeneration of damaged tissue by bone marrow mesenchymal stem cells, and of “Regeneration-Inducing Medicine™”, we have continued research focused on cells in their natural state found in the body, such as mesenchymal stem cells present in bone marrow, mesenchymal stem cells present in blood flow and mesenchymal stem cells present in damaged tissue. We are accelerating our research into “Regeneration-Inducing Medicine™” based on these findings by combining them with newly developed screening methods for mobilization of mesenchymal stem cells into blood.
As a result of the above basic research, we have continued to collect new findings relating to bone marrow mesenchymal stem cells present in the body, and have obtained a substance that mobilizes new bone marrow mesenchymal stem cells into the blood. As with PJ1, this is expected to become a “Regeneration-Inducing Medicine™” for a wide range of diseases involving tissue damage. As well as biologic peptides, we are also developing peptides prepared based on information about biologic activated peptides.
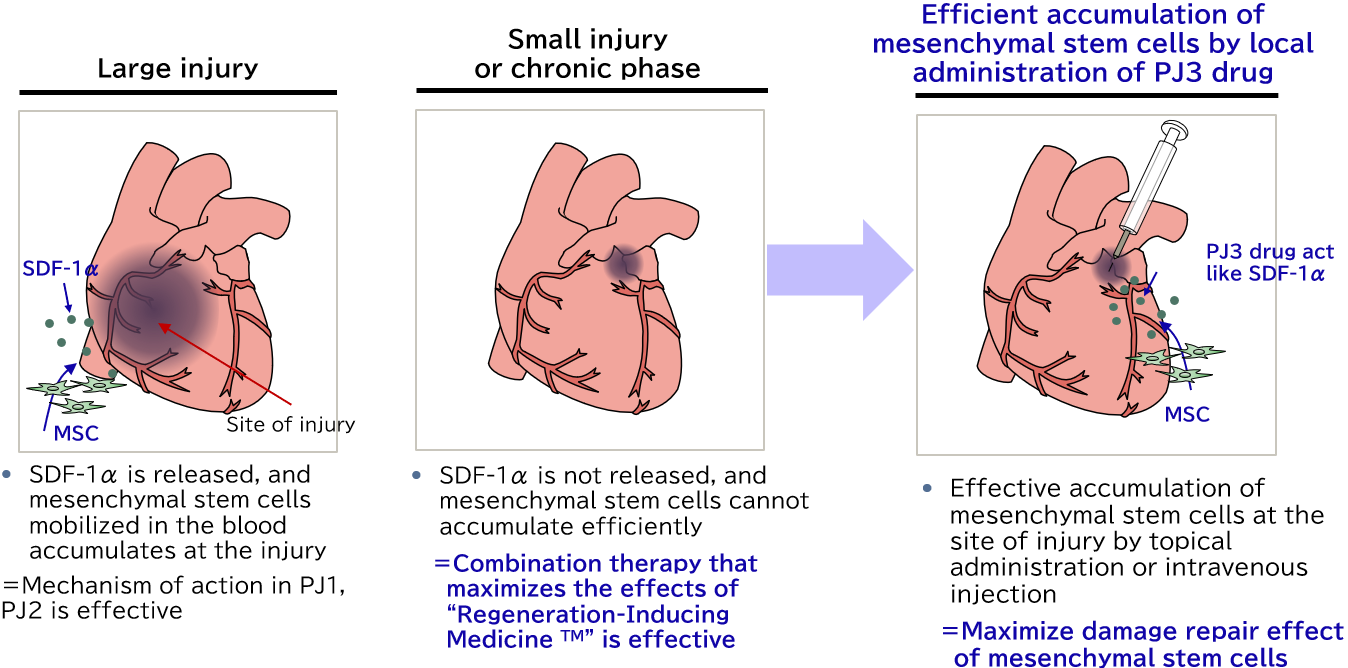
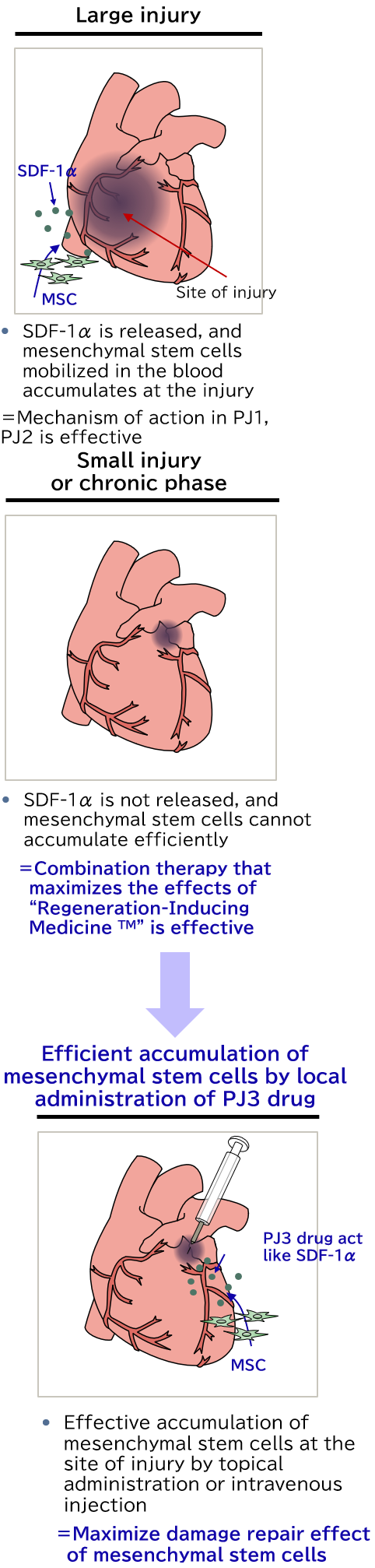
PJ3: Novel Regeneration-Inducing Peptide for Local administration
These are protein preparations derived from proteins in the body extracted from living tissue. When administered intravenously or locally, they efficiently accumulate the mesenchymal stem cells in the body to the affected site, and are expected to become therapeutic medicines for a wide range of diseases involving tissue damage.
The products being developed in PJ1 and PJ2 are substances that stimulate mesenchymal stem cells in the bone marrow, mobilizing the mesenchymal stem cells from the bone marrow into the blood. In PJ3, however, we are developing a substance that increases the secretion of substances mobilizing mesenchymal stem cells from the damaged tissue.
Since the mechanism of action of these substances is different from that of HMGB1 peptides, their use, either in combination with HMGB1 peptides or as monotherapy, is expected to expand the range of target diseases of regeneration-inducing therapy. In particular, in conditions with a small amount of damaged tissue, the region of ischemia is small, and so there is a small amount of SDF-1α increasing the amount of secretion in a hypoxic state, and thus there is a risk that mesenchymal stem cells may not accumulate at the damaged location. In a situation like this, this substance can be administered to the periphery of the affected site, with the aim of accumulating mesenchymal stem cells in blood circulation to the organ being treated.